A birthing pool is a large portable or fixed pool of warm water used during labour and, in many cases, for the birth itself. Used in NHS hospitals, midwife-led birthing centres, and home births across the UK, they are one of the most commonly requested forms of pain relief in labour — and one of the few for which there is now a large and reassuring body of evidence on both maternal and neonatal outcomes. This guide covers how birthing pools work, what the evidence says about their benefits and risks, and what to know if you are considering hiring or buying one for a home birth.
- NICE 2025 guidance states every pregnant woman has the right to ask for and should be offered the option to labour in water
- The UK POOL cohort study (2024, NIHR) found adverse neonatal outcomes were no higher in waterbirth than land birth: 2.7% vs 4.4%
- Cord avulsion (umbilical cord snapping) is more common in waterbirth — 4.3 per 1,000 vs 1.3 per 1,000 on land — but no babies with this complication died in the POOL study
- Recommended water temperature is 37°C at birth, never exceeding 37.5°C; NHS trusts check temperature hourly
What Is a Birthing Pool and How Does It Work?

Hospital birthing pools and midwife-led units
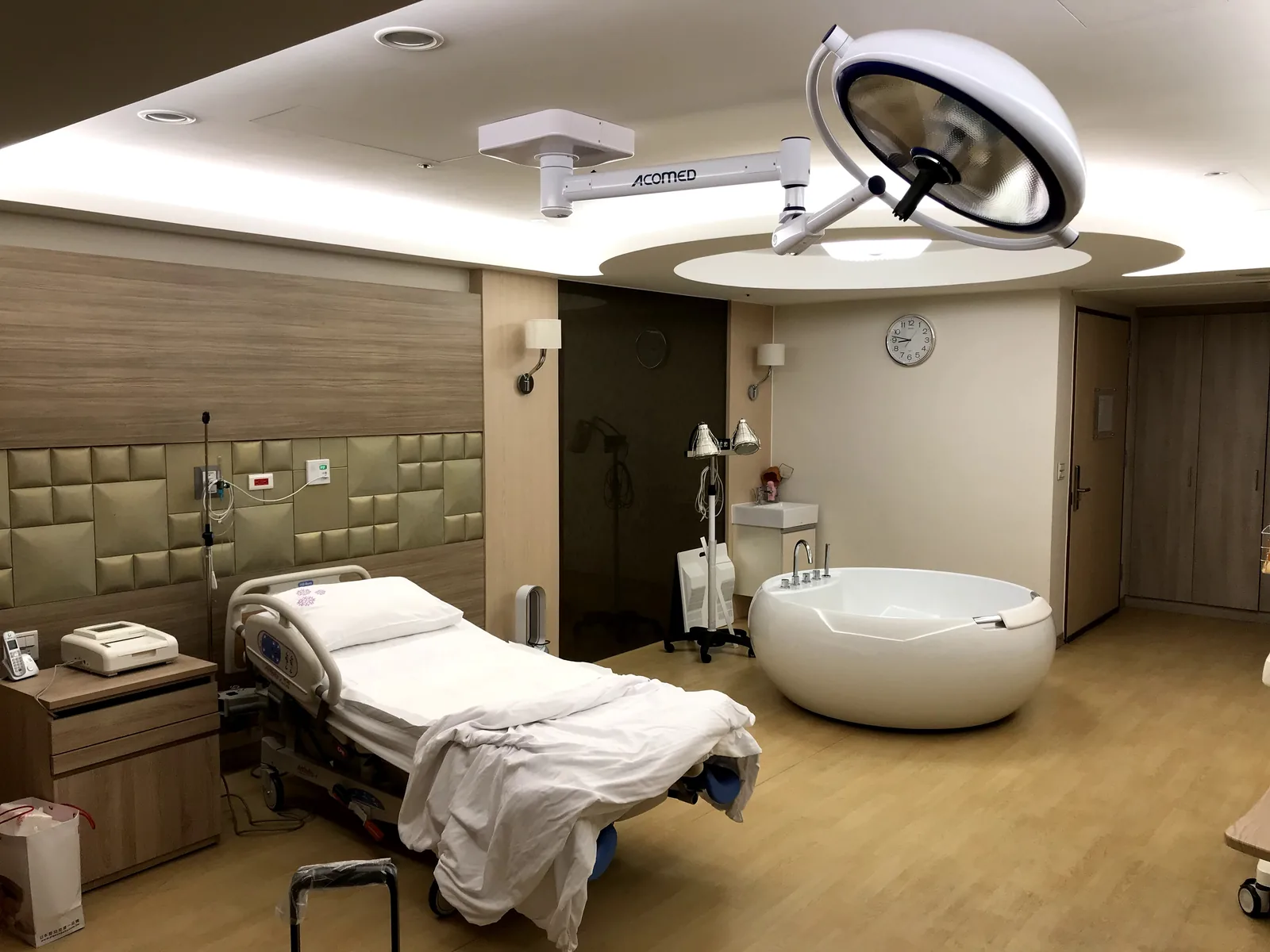
Most NHS labour wards and midwife-led birthing centres now have at least one fixed birthing pool available. These are large, purpose-built baths — typically 1.5–2 metres in diameter and deep enough to allow full submersion of the abdomen in a seated or kneeling position. Hospital pools are fed from direct hot and cold water supplies, maintained at the recommended temperature, and emptied and thoroughly disinfected between uses. There is no additional cost to use an NHS birthing pool, but they cannot be booked in advance: availability depends on the pool being free and clean at the time of arrival in labour.
NCT guidance on water birth notes that not all NHS hospitals have pools, and even those that do may not always have one available. Midwife-led units (MLUs) typically have better pool availability than standard obstetric units. If a birthing pool is central to your birth plan, confirm pool availability with your midwife team and understand what happens if the pool is in use when you arrive.
Temperature, hygiene, and practical setup
The recommended water temperature for a birthing pool is 35–37°C during the first stage of labour and 37°C for the birth itself. Water should never exceed 37.5°C — higher temperatures can raise the baby’s core temperature and increase neonatal heart rate, creating a risk of distress. NHS trusts check water temperature hourly and adjust it to keep the mother comfortable within safe limits. A waterproof thermometer is essential equipment for home births.
Hygiene is a significant consideration, particularly for home births. Public Health England guidance on home birthing pools specifically warns against pre-filling the pool and maintaining temperature with a heater or pump before labour begins, due to the risk of Legionella bacteria growing in warm stagnant water. The pool should be filled with fresh water as close to the start of active labour as possible, using a dedicated clean hose. If using a hired pool, the liner should be new and unused for each birth.
Who is eligible for a water birth
NHS eligibility criteria for birthing pool use are consistent across most trusts. Typically, a woman can use a birthing pool if she has had an uncomplicated pregnancy, is between 37 and 42 weeks, is carrying a single baby in a cephalic (head-down) presentation, has a BMI of 35 or below, and can get in and out of the pool independently. Women who have had an epidural cannot use a birthing pool as the epidural prevents feeling in the legs, making safe movement in and out impossible. Medical complications — previous caesarean, certain fetal monitoring requirements, Group B Streptococcus (GBS) colonisation in some trusts, or bleeding — may also restrict access.
NICE guidelines updated in 2025 state that every pregnant woman and birthing person has the right to ask for and should be offered the option to labour in water, reflecting a shift toward supporting water immersion as a standard choice rather than a special request.
Benefits and Risks of Birthing Pools — What the Evidence Says
Pain relief, mobility, and maternal benefits
The pain relief benefits of water immersion in labour are the primary reason most women request a birthing pool. Warm water has a well-established analgesic effect: it reduces the body’s production of stress hormones (adrenaline and noradrenaline) and supports the release of endorphins, the body’s natural pain-relieving compounds. The buoyancy of the water allows a near-weightless feeling that makes it easier to adopt comfortable positions, change position frequently, and use gravity effectively in labour — all of which support progress. Women who labour in water consistently report feeling more in control and less reliant on pharmacological pain relief.
Evidence on maternal outcomes is favourable. A 2023 systematic review and meta-analysis in the American Journal of Obstetrics and Gynecology found that waterbirth was associated with a 20% reduction in postpartum haemorrhage risk and a 31% reduction in low Apgar scores. The water’s warmth supports perineal tissue stretching and relaxation, which may reduce the need for episiotomy.
Neonatal outcomes and the cord avulsion risk
The largest and most recent study of waterbirth outcomes in the UK is the POOL cohort study, funded by the NIHR and published in 2024. The study followed nearly 15,000 births across 26 NHS sites. Adverse neonatal outcomes occurred in 2.7% of waterbirths compared to 4.4% of land births — not higher in the water group. Baby deaths were rare in both groups: 2 per 10,000 waterbirths and 3 per 10,000 land births. Neonatal aspiration was 40% lower and NICU admission 44% lower in the waterbirth group.
The one risk that is meaningfully higher in waterbirth is cord avulsion — the umbilical cord snapping before it is clamped. This occurred in 4.3 per 1,000 waterbirths compared to 1.3 per 1,000 land births (approximately three times more common). The mechanism is thought to involve the baby moving more freely in the water after delivery, increasing tension on the cord before the midwife can clamp it. Importantly, in the POOL study, no babies who experienced cord avulsion died, and none required therapeutic hypothermia or blood transfusion. However, cord avulsion is a known and specific risk of waterbirth that midwives are trained to anticipate and respond to.
Infection risk and home pool safety
Neonatal infection rates were 36% lower in waterbirths than land births in the POOL study — a counterintuitive finding given concerns about water contamination. This is likely explained by the reduced use of invasive interventions (internal monitoring, augmentation) and fewer perineal tears in water births, rather than any antimicrobial property of the water itself. For home births, infection risk is managed by ensuring the pool liner is new, the water is freshly filled immediately before use, and the pool is not pre-filled and maintained at temperature for extended periods — the conditions most associated with Legionella risk in domestic water systems.
Hiring or Buying a Birthing Pool for a Home Birth

Pool types and costs
For women planning a home birth, a birthing pool must be arranged privately unless the local NHS trust provides one on loan (some do — check with your community midwifery team). The main options are purchasing or hiring. Purpose-built inflatable birth pools — designed with deeper sides, more rigidity, and appropriate dimensions for safe use during labour — are available to buy from around £150–£250 from specialist suppliers such as Barefoot Birth Pools and similar UK retailers. Hire packages including the pool, a new disposable liner, hose, and pump typically cost £80–£150 for a 4–6 week hire period, which covers the period around the due date. A new liner (£20–£35), tap connector hose (£15–£25), and a waterproof thermometer are the essential additional items.
Semi-rigid and hard-sided birth pools are also available and offer better temperature retention than fully inflatable models — important for a home birth where maintaining the correct temperature manually is harder than in hospital. These typically cost £300–£600 to purchase and are suitable for multiple uses with a new liner each time.
Setting up a home birthing pool safely
Setting up a home birthing pool involves several practical considerations beyond the pool itself. The weight of a filled pool — a standard birth pool holds approximately 500–700 litres — means that floor strength must be considered, particularly for upper-floor rooms. Water volume and outlet access are also relevant: filling and emptying a 600-litre pool requires a hose connection to a tap or bath mixer (a standard mixer tap adaptor is included in most hire kits) and a submersible pump for emptying. Waterproofing the floor beneath the pool with plastic sheeting prevents water damage from splashes and the birth itself.
Midwives attending a home birth will assess the setup before labour progresses to the pool stage. They will bring equipment to monitor the baby’s heart rate electronically from outside the pool (waterproof Doppler monitors) and will need clear access to both sides of the pool for safe attendance of the birth.
For information on other types of pools and water environments, see our guide to outdoor swimming pools and lidos in the UK. For context on pool water safety and infection risks more broadly, our article on swimming pools and UTIs covers the evidence on water-borne infection in recreational swimming.
Frequently Asked Questions
Are birthing pools safe for the baby?
Yes — the evidence from the UK POOL cohort study (2024, NIHR) shows that adverse neonatal outcomes are no higher in waterbirth than land birth (2.7% vs 4.4%). Baby deaths are rare and similar in both groups. The one specific risk that is higher is cord avulsion (umbilical cord snapping before clamping), which occurs around three times more frequently in waterbirths — but no babies with this complication died in the POOL study. Midwives are trained to manage this risk.
Can I have a water birth at an NHS hospital?
Yes, if your hospital or midwife-led unit has a birthing pool and one is available when you arrive in labour. NHS pools are free to use. They cannot be booked in advance, and availability is not guaranteed. NICE 2025 guidance states that every pregnant woman should be offered the option to labour in water. Contact your midwifery team to find out whether your unit has a pool and its typical availability.
What temperature should a birthing pool be?
35–37°C during the first stage of labour, and 37°C for the birth itself. The temperature should not exceed 37.5°C at any point, as higher temperatures risk elevating the baby’s core temperature. NHS midwives check and record pool temperature hourly. For home births, a reliable waterproof thermometer is essential — check temperature every 15–30 minutes and add cold water to cool it if needed.
How much does it cost to hire a birthing pool for a home birth?
Hiring a birthing pool for a home birth typically costs £80–£150 for a 4–6 week hire period, including the pool, a disposable liner, hose, and pump. Purchasing a dedicated birth pool outright costs £150–£600 depending on whether it is fully inflatable or semi-rigid. Additional items needed include a tap adaptor hose (£15–£25), a new liner if not included (£20–£35), and a waterproof thermometer. Some NHS trusts offer birth pool loan schemes — ask your community midwifery team.
What are the risks of using a birthing pool at home?
The main additional risks at home compared to hospital include: Legionella risk if the pool is pre-filled and temperature-maintained for hours before labour (fill fresh immediately before use); temperature management without automated systems (check regularly, never exceed 37.5°C); and the fact that if complications arise, emergency care is not immediately available. Home births are recommended for low-risk pregnancies only. Your midwifery team will assess whether a home water birth is appropriate for your circumstances.



